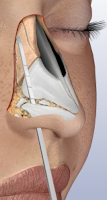
By now those of you who have been following this site, will be aware of the terms external and internal nasal valve collapse. When thinking of those terms we automatically think of lateral collapsing of the nasal wall towards the septum particularly with inspiration. But when a significant amount of your tip cartilage (the middle and medial crura) are excised during rhinoplasty you will likely notice, as is in my case, that your nostrils are now significantly less projected then they were before your primary nose surgery. In fact the short projection of my nostrils were pointed out to me by a revision rhinoplasty surgeon a few months back. At closer inspection of the base view of my nostrils, I would guesstimate (since i don't have nostril pictures of my original adult pre-operated nose) that my nostrils are close to half the length of what my nostril projection was prior to my primary surgery. I have had my tip reduced in all of my three revision rhinoplastys, as well as reduced and reshaped in my primary. My nasal spine was also reduced in one of my revisions. The problem of an overly large nasal tip was a result of my primary nose surgeon being overly aggressive with my bridge (I had a very large hooked shaped nose), so by overcompensating for that, the surgeon ended up giving me a ski sloped nose with a very long protruding tip... the Cyrano effect A big cosmetic assessment mistake that was made by my last surgeon was not understanding how to safely bring into balance the longer tip with my scooped out bridge. The safe, smarter but more complex procedure which should have been performed, was to add grafts to my bridge building it up to line up better with my tip. Another possibility which could of been performed alone or in tandem with the former was to reshape the tip cartilages using sutures and rotate it downward, since I already had some excision to my tip cartilages previously. Unfortunately the surgeon wasn't that experienced or skilled so he decided to opt for quick & easy 'fix' and aggressively excise the tip cartilages further down, not taking into account all the previous excisions i had. So in essence he was able to achieve the cosmetic goal of reducing the length of my tip, but unfortunately not without major consequences. I don't believe I have tip ptosis at least not a very distinguishable form of it because my tip was already positioned fairly high after my first revision surgery. However it's very likely that the major and minor supporting tip structures have been negatively impacted on, as well as the vascularity of my skin and soft tissue envelope. I would assume that in order to correct my flattened "shrunk" nostrils i would probably require tip projection as well as correcting the lateral collapse I have, to achieve a normal and relatively proportional sized nostrils ( proper ratio's) for the base of my nose. It's also important to recognize that anything which decreases the nasal valve cross sectional area can negatively impact the nasal airway, creating further feeling of nasal obstruction. Even though there's a significant amount of information about reducing flared out nostrils for cosmetic reasons, not much exists for increasing or restoring the size of one's flattened out nostrils due to prior nose surgery's. At least not that I have found online. As far as nasal tip ptosis is concerned I will discuss that in greater detail on another post.
.
Motivation for this blog: To have a major resource center that will better inform those considering revision rhinoplasty in order to make well informed decisions; based on my own personal experiences as a nose revision patient, as well as my research.
Friday, December 21, 2012
Tuesday, October 23, 2012
Growing nasal cartilage in the lab: Engineering of autologous septal cartilage
Well the possibility for those who need extra nasal cartilage in the nose for aesthetic or functional reasons but don't have enough existing nose cartilage, may soon have another option. On a previous post titled, "Regenerative medicine:Re-growing body parts" August 28 2010 I posted a video discussing in particular how a man was able to regrow his finger using a powder, and it discusses tissue engineering in general, however not for nose in particular. For those that haven't yet read my previous posts; harvesting cartilage from your own body is preferred method of choice for replacing, or strengthening missing or weakened cartilage in the nose. For the nose, the gold standard is nasal cartilage from the quadrilateral region of the septum. When there isn't enough remaining cartilage there because of previous surgical removal the surgeon can harvest cartilage or bone from, ribs, ears, cranium, or hips. Other sources can be from cadaver, or use of synthetic materials. All these are inferior choices to your own nasal cartilage and have their own unique set of drawbacks. However if cells from your nasal cartilage can be isolated and grown in a lab, to grow new cartilage then that would be the ideal. This research has been underway for couple years now at UC San Diego!
"Researchers at UC San Diego have turned to tissue engineering to develop replacement cartilage for the nose. Dr. Deborah Watson says a small amount of cartilage is removed from the patient’s nose. Technicians isolate the cells from the tissue, then grow the cells to increase their number. The cells are then placed into a three-dimensional matrix, where they will continue to grow in number and form tissue. Enzymes and growth factors are added to encourage growth and formation of a harder tissue.
Watson says it can take two to three months to generate cartilage that is strong enough to place back in the body. The surgeon will fine tune the shape of the cartilage before inserting it back into the nose. The “new” cartilage is either placed inside a pocket of soft tissue or sutured to remaining cartilage in the nose. Once in place, the engineered cartilage will continue to mature and become stronger.
Cartilage tissue engineering is still in testing phases and not yet approved by the FDA. Watson says the process may eventually enable doctors to provide patients who need nasal reconstruction with an aesthetically pleasing and functional nose. Since the cells come from the patient’s own body, theoretically, there is no risk of rejection of the engineered cartilage."
http://www.wsoctv.com/news/news/health-med-fit-science/growing-noses/nG9ST/
http://www.webmd.com/healthy-beauty/video/growing-noses
©noserevisionsurgeryandsurgeons.blogspot.ca
I really hope that researchers will soon conduct tissue engineering of the turbinates as well, for those who suffer from Empty Nose Syndrome. Except for parts of the sexual organs, which is not an option as donor site, there really is no other part of the human body that acts like or resembles the natural vascularness of the turbinates to be used for replacing lost tissue due to over resectioning.
http://emptynosesyndrome.org/what_is_ens.php
Monday, October 22, 2012
Is there a point where it makes more sense to replace & rebuild the entire alar (lower) nasal cartilage?
At one of my nose revision consults, a well known facial plastic surgeon commented to me how he has removed many grafts from patients noses, because they were over-grafted, leaving the nose too bulky & esthetically unpleasing. He also said he has a rule that when more then 50% of the cartilage is missing (normally due to excessive removal from previous surgery) he decides to replace the whole thing, which although is more time consuming and requires more precise measuring results in a much more natural looking and functional nose compared to adding a variety of different sized grafts to the existing residual nose cartilage throughout the nose. I assume that if the remaining cartilage is of poor quality or too small it would be comparable to a weak foundation therefore affecting the stability & position of newly grafted cartilage anchored and extending from it. He had shown me before/after pictures of such cases and there was no question the results of his work was an improvement.
Since no other surgeon ever mentioned this to me I began to search online to see if this rule has been documented by other surgeons. While, I didn't find anything that specifically mentions this rule in regards to lower or upper cartilage of the nose, I did find this rule has been applied to when more then 50% of a subunit of the nose is missing. Here is what i was able to find.
"In modern times, the practice of reconstruction has been advanced by the work of surgeons such as Burget and Menick,' who proposed the subunit principle of nasal reconstruction. They found that changes in soft tissue and bony contours of the nose resulted in distinct, consistent nasal subunits, including the dorsum, tip, columella, 2 lateral side walls, 2 alae, and 2 soft tissue triangles! These authors found that if greater than 50% of an aesthetic subunit of the nose were missing, it was better to resect the rest of the subunit and reconstruct it in its entirety."
"In 1985, they published the first in a series of articles applying the subunit concept to nasal reconstruction.' In patients with 50% or greater subunit losses, these authors performed esthetically superior reconstruction by removing the remaining portion of the subunit and reconstructing the entire subunit with a skin graft or flap. Burget and Menick later supported the principle of subunit nasal reconstruction and emphasized that like tissue should be replaced by like tissue."
In regards to specifically replacing the entire alar cartilage (lower nasal cartilage) the only thing that I was able to find was something I had discussed a long while ago in my post on 'The mystery of all those different nose grafts (Oct 18,2010)" which was the seagull wing graft. However the criteria for determining the decision to replace the alar cartilage with this replacement graft seems to be determined differently then the 50% rule, but not necessarily since the author doesn't mention what amount constitutes "severe signs of overresection...". He states: "The seagull wing technique is indicated in cases in which there are severe signs of overresection of the lower lateral cartilages. Usually, it is recommended for patients who present with a variety of aesthetic and functional complaints, eg, insufficiency of the external nasal valve, alar pinch, or an an intraoperative diagnosis of overresected lower lateral cartilages. In most cases, these indications are associated with poor tip definition and projection and alar retraction. The technique can also be used to lengthen an overrotated and short nose."
Since the nasal tip subunit consists of the alar lower cartilage, perhaps this is why that surgeon i had seen applies the 50% rule.
If any surgeon reading this blog has more knowledge to add to this subject please feel free to contact me or leave a comment.
©noserevisionsurgeryandsurgeons.blogspot.ca
Sources:
http://www.drsherris.com/articles-and-research/esthetic-refinements
http://archfaci.jamanetwork.com/article.aspx?articleid=481047
Update: Dec 21, 2012
another link to view
http://www.drmenick.com/wp-content/uploads/2012/06/PDF%20Anatomic%20Reconstruction%20of%20the%20Nasal%20Tip%20Cartilages%20in%20SecondaryReconstructive%20Rhinoplasty.pdf
Since no other surgeon ever mentioned this to me I began to search online to see if this rule has been documented by other surgeons. While, I didn't find anything that specifically mentions this rule in regards to lower or upper cartilage of the nose, I did find this rule has been applied to when more then 50% of a subunit of the nose is missing. Here is what i was able to find.
"In modern times, the practice of reconstruction has been advanced by the work of surgeons such as Burget and Menick,' who proposed the subunit principle of nasal reconstruction. They found that changes in soft tissue and bony contours of the nose resulted in distinct, consistent nasal subunits, including the dorsum, tip, columella, 2 lateral side walls, 2 alae, and 2 soft tissue triangles! These authors found that if greater than 50% of an aesthetic subunit of the nose were missing, it was better to resect the rest of the subunit and reconstruct it in its entirety."
"In 1985, they published the first in a series of articles applying the subunit concept to nasal reconstruction.' In patients with 50% or greater subunit losses, these authors performed esthetically superior reconstruction by removing the remaining portion of the subunit and reconstructing the entire subunit with a skin graft or flap. Burget and Menick later supported the principle of subunit nasal reconstruction and emphasized that like tissue should be replaced by like tissue."
In regards to specifically replacing the entire alar cartilage (lower nasal cartilage) the only thing that I was able to find was something I had discussed a long while ago in my post on 'The mystery of all those different nose grafts (Oct 18,2010)" which was the seagull wing graft. However the criteria for determining the decision to replace the alar cartilage with this replacement graft seems to be determined differently then the 50% rule, but not necessarily since the author doesn't mention what amount constitutes "severe signs of overresection...". He states: "The seagull wing technique is indicated in cases in which there are severe signs of overresection of the lower lateral cartilages. Usually, it is recommended for patients who present with a variety of aesthetic and functional complaints, eg, insufficiency of the external nasal valve, alar pinch, or an an intraoperative diagnosis of overresected lower lateral cartilages. In most cases, these indications are associated with poor tip definition and projection and alar retraction. The technique can also be used to lengthen an overrotated and short nose."
Since the nasal tip subunit consists of the alar lower cartilage, perhaps this is why that surgeon i had seen applies the 50% rule.
If any surgeon reading this blog has more knowledge to add to this subject please feel free to contact me or leave a comment.
©noserevisionsurgeryandsurgeons.blogspot.ca
Sources:
http://www.drsherris.com/articles-and-research/esthetic-refinements
http://archfaci.jamanetwork.com/article.aspx?articleid=481047
Update: Dec 21, 2012
another link to view
http://www.drmenick.com/wp-content/uploads/2012/06/PDF%20Anatomic%20Reconstruction%20of%20the%20Nasal%20Tip%20Cartilages%20in%20SecondaryReconstructive%20Rhinoplasty.pdf
Tuesday, July 10, 2012
Sources and sites used for constructing nasal grafts: Generally accepted principles
 |
| Decision Tree (algorithm) for revision rhinoplasty [4] |
*** NOTE: DICED RIB CARTILAGE IS NOT MEANT FOR STRUCTURAL SUPPORT. ie. spreader, lateral crura strut or batten graft. FOR THAT YOU NEED SOMETHING STRONGER LIKE SOLID PIECE OF SEPTAL, OR RIB CARTILAGE FOR THOSE NEEDING STRONG SUPPORT. EAR CARTILAGE IS USED MORE IN THE LOWER THIRD OF THE NOSE AND FOR CASES THAT DON'T REQUIRE STRONG SUPPORT. THIS IS VERY SUBJECTIVE AND WHERE SURGEONS HAVE VARYING OPINIONS ABOUT LOCATION OF HARVESTING THE GRAFT.
So as you can see our own personal circumstance also weighs in quite heavily when the surgeon decides which grafts will be used and which won't. Another major factor as to what a surgeon will prescribe for grafting depends on his/her level of expertise and training. Some nose surgeons were never trained to harvest autologous body grafts therefore prefer to restrict their use to synthetic implants or cadaver (homologous grafts) , some have no experience with synthetic grafts and limit their practice to auto and allografts, some only septal and ear, and very few will have experience with many different types of autologous grafts and will eventually specialize in using some of the following; septal, ear, rib, calvarial bone, Iliac crest grafts, diced with fascia, crushed cartilage, composite grafts, and soft tissue grafts. Not only is there differing opinions about the material composition of the graft to use, but as well as to the actual TYPE of graft to use. ie. In case of increasing Lateral support to correct Nasal Valve Collapse, some will recommend Lateral crural strut graft, some prefer Alar or Sub-Alar batten graft, some like Butterfly graft, or may recommend a Spanning Alar graft. Specific indicators after thorough examination of the overall nose & being cognizant of what the desired goals are, the surgeon will determine which type of graft would be most appropriate. With experience surgeons will become more proficient and favor certain methods over others, some even modifying &/or developing new procedures. For those that are younger and have never had septal cartilage removed, you are in superior position (assuming all is equal) for revision nose surgery, compared to someone who is over middle age and no septal cartilage to work with.
Some patients online have claimed that when they had costal cartilage in the columellar there smile was negatively affected. That however could be due to improper placement or size of the graft, being too wide or long. If too large of a solid graft is used in tip area, there will be increase risk of extrusion and/or skin necrosis.
Some surgeons also seem more proficient with sutures while others are more adept at grafting. ex.. An alternative for alar batten grafts is the Lateral crus pull-up. It is a suture technique in which the lateral crus is pulled up laterally and upward to the bony pyramid. The effect is twofold widening of the valve area and strengthening of the lateral wall [3]. In some cases instead of using a Lateral crura strut graft, the cephalic lateral crus can be reorientated to give support and correct aesthetic defects. Gruber et al [5]created an “island” of cephalic lateral crus that was slipped under the main body of the lateral crus to stiffen and straighten it. They suggest that the cephalic part of the lateral crus can act as a lateral crural strut to maintain the ala in a more caudal position Tongue in groove is another popular suture technique used to aid in correction of columellar show, a deviated caudal septum, and various tip rotation and projection problems. It is typically used in combination with other septorhinoplasty maneuve. Many surgeons utilize both grafting and complicated suture techniques during surgery for optimal cosmetic and structural results.
It can be very daunting task to figure all this out and getting opinions online like on realself.com which is a great site, demonstrates how widely surgeons opinions and approaches vary, sometimes even contradicting each other. As in the example in dorsal augmentation there are many choices (autografts; bone, solid or diced cartilage, soft tissue, homografts, alloplasts,) available to choose from as I mentioned earlier. Beware though, that in some cases the surgeons are not simply contradicting each other, but suggesting a better alternative to correct specific problem(s) for specific type of individuals. Some surgeons will use whats called superficial muscular aponeurotic system. (SMAS) graft.(more applicable and useful for those with THICK SKIN) which is an autologous soft tissue filler onlay graft, while others may use crushed cartilage for onlay graft. Some nose surgeons recommend Fascia Lata over bone grafts in dorsal augmentation because it's a heavier fascia which is better to conceal the rigidity of a bone graft. Some may suggest Lateral crural strut graft because it corrects few problems at once, like narrowing a bulbous tip, and strengthening a weakened nasal valve. A competent revision nose surgeon will be knowledgeable and able to perform many types of grafts, sutures, flaps, and other septorhinoplasty modifying techniques [I.E. Lateral crural steal (LCS) & Lateral crural overlay (LCO)/Medial crural overlay (MCO)]and know which alternative method to apply according to each individual's specific case. What they discover esp. in revision rhinoplasty during surgery may justifiably cause them to alter or add/subtract to their pre-surgical plans. A good surgeon should be prepared for worse then expected scenarios. ie. during surgery the surgeon discovers that the patient's lower cartilages need to be reshaped, repositioned, or totally replaced with new cartilage.
 | |
| This algorithm (above) reflects Dr.W.H..Beeson's preferences |
Generally Accepted Principles for Nasal grafting:
1. Your own body is best source for grafts (bone,cartilage, soft tissue). Referred to as Autografts also known as Autogeneous, Autologous grafts. Best site within your body for nose grafts, is the septum. If there isn't enough septal cartilage, then other options are; Rib, Ear, or Calvarial as mentioned above.
2. Allografts/Homografts/Homologous-irradiated(cadaver grafts) are another good source for cartilage but work better in the immobile regions of nose.Alloderm (skin cadaver graft) has high absorption rate.
3. Synthetic implants (Alloplasts) Types: Silicone, Meshed, Porous, Porous high density polyethylene (PHDPE;Medpor),Expanded polytetraflouroethylene (e-PTFE ;GoreTex). Which is preferred is debatable amongst surgeons. GoreTex seems to be best of the choices, but some like Medpor. Silicone/Silastic implant which has been used extensively in Asian rhinoplasty is losing favor due to high rates of infections and extrusions. Meshed are also not favored due to infection rates. Medpor can be a problem when needed to be removed due to it's modest porosity. Higher porosity values means it integrates more with surrounding tissue therefore more difficult to remove without causing more damage or removal of surrounding tissue. This is why GoreTex may be preferred since it has a low porosity value. Silicone has no porosity so remains separated and unfixed. It however carry's significant risk of extrusion, higher in columellar area then dorsal area, and is not meant for structural support.
4. Xenografts is from another species mostly from bovine (cattle) or porcine (pigs). Eg. Enduragen is a tough but flexible biomaterial made up of cross-linked porcine dermal collagen and its constituent elastin fibers. Its use is indicated for tissue augmentation of the head and face, and it is commercially available in flat sheets. Permacol is another type made by different manufacturer. There is risk of allergic reaction to such type of material. To my knowledge not commonly used in Nasal revision surgery.
5. Soft tissue filler is normally preferred from own body. ex. fascia grafts
6. Bone graft, like cartilage, can be used for augmentation and as a supportive structural framework for nasal tip and internal nasal valve support. Generally considered a second choice after autogenous cartilage.
Note: In every case the Surgeon has to weight the pros/cons so their may be justifiable exceptions to the above list. Important that the surgeon & patient discuss all the options which relate to the patient's circumstances.
Open Approach to nose surgery has become more popular allowing clear visual inspection, ease of access to existing structures, & allowance for implanting larger sized grafts. This could lead however to more unnecessary over grafting of the nose. Closed Approach advantages are no scarring, less dissection which is important for those who have had prior nose surgery therefore less damage to soft tissue,vascular, & innervation system of the nose, and faster healing period. More conservative methods are being employed today compared to past, where a lot of reductive surgery was performed, without taking into account supporting structure of the nose.Today astute nose surgeons are even placing grafts in some primary surgery's to avoid long term pitfalls.
Future:
- Preserved cartilage for future surgery. Primary & Revision patients should request for their surgeons to preserve cartilage that may be removed and not re-used during the surgery.
- Tissue engineering
***Here's an excellent slideshow you should watch: ***
This slideshow called Grafts in Nasal Surgery by Dr. D.J.Menger What I really like about it, is how he mentions in some cases his preference of cartilage grafts. He doesn't mention synthetic material, so I gather that would be his last preference.http://www.slideshare.net/therhinoplastycourse/grafts-in-nasal-surgery
©noserevisionsurgeryandsurgeons.blogspot.ca
Interesting site's to look at:
http://www.egms.de/static/en/journals/cto/2011-9/cto000065.shtml
http://www.shimmianmanila.com/side-effects-of-silicone-implant
References;
[1] Menger D.J., Fokkens W.J., Lohuis P.J., Ingels K.J., Nolst Trenité G.J. Reconstructive surgery of the leprosy nose: a new approach. J Plast Reconstr Aesthet Surg. 60(2):152-62, 2007
[2] http://www.realself.com/question/Best-material-nose-implant
[3] Grafts in Nasal Surgery p.77 D.J.Menger
[4] Chapter 30: Revision Surgery in Otolaryngology by David Edelstein
[5] Gruber RP, Zhang AY, Mohebali K. Preventing alar retraction by preservation of the lateral crus. Plast Reconstr Surg. 2010;126(2):581-5
Tuesday, July 3, 2012
Osteotomies In Nasal Surgery
 | |
| Lateral osteotomy |
 | |
| medial osteotomy |
Osteotomy is a term used to describe surgical procedures during which bone is divided, or a piece of bone is cut off. In most rhinoplasty procedures, some form of osteotomy is usually required, to move or modify the osseocartilaginous vault, which comprises a major part of the nose.
In rhinoplasty, osteotomy may involve the 'excising' or 'breaking' of bones in the nose. It is usually performed to correct a nasal hump, enhance a twisted nose, or make a wide nose narrower
The bony portion (the top 1/3 portion of the nose) is referred to as "the bony vault." According to Oneal, Izenberg, and Schlesinger, "[It] … consists of the paired nasal bones and the frontal ascending processes of the maxilla. The vault is generally pyramidal in shape
The nasal bone can generally be moved only after it has been carefully cut from the tissue and cartilage around it. This is usually done with the help of sharp chisels, which may be introduced either from the inside of the nose, or through a small incision made at the side. The surgeon performing this procedure needs to possess a high level of skill, to ensure minimal damage to the nasal lining, and reduce post-operative swelling and discomfort.
Different types of nasal osteotomies performed are: 1. Paramedian (medial) osteotomy 2. Lateral osteotomy 3.Transverse osteotomy 4. Intermediate osteotomy and 5. Oblique osteotomy.
One of the common osteotomic approaches used in nose surgery is the medial osteotomy. During this type of osteotomy, the nasal bone is cut in the middle with a 'back cut'. Then, a small osteotome (bone knife) is positioned along the edge of the bone, and gently tapped to move it along a previously planned path. After the bone is cut, it can be moved, as required. The indications for medial osteotomy are: 1.When mobilization of the entire sidewall is recommended.2. To help prevent uncontrolled or irregular back-fracture from the upper portion of a lateral osteotomy. 3. To widen an overly narrowed bony nasal vault.
Lateral osteotomy is used to close a nasal dorsum (open roof) and to narrow or straighten the nasal pyramid.
Complications of lateral osteotomy, include: infection, bleeding, massive edema, anosmia, lacrimal duct injury, intracranial injuries, disfigured appearance, narrow airway and nasal obstruction. Note: Lateral osteotomy with infracture can cause the nasal valve angle to be too narrow. Valve angle (nasal breathing) is compromised when it is less then 10 to 15 degrees.
An osteotomy between the medial and lateral osteotomies is occasionally indicated. The primary use's of Intermediate osteotomies are:: 1. To narrow the extremely wide nose that has good height (bilateral osteotomy). 2. To correct the deviated nose with one side wall much longer then the other. To correct a deviated nose sequential osteotomies are performed in a fashion similar to opening a book. 3. To correct the abnormally contoured nasal bone that is either excessively convex or concave. Intermediate osteotomies are most effective for decreasing the curvature of an excessively convex nasal bone. The intermediate osteotomy allows recontouring of the nasal bone for correction of the severely deviated bony vault. This osteotomy is performed before the lateral osteotomy.
NOTE: This process of breaking the bone and resetting it to narrow the nose is called an infracture. If the nose is being widened after the nasal bones are broken, it is called an outfracture.
Complications of bony pyramid and osteotomies: See my post on "Complications of Rhinoplasty"Dec.11, 2011 sections: Collapse of bony pyramid, Osteotomy complications and Upper Third deformities. Also my post titled: "Does a narrowing of the nasal passage-way simply mean correcting the collapsed valve region with cartilage grafts?"Jan. 29, 2012
Note: Straightening and narrowing the upper third of the nose doesn't mean a crooked nose will then be straight. The remaining 2/3rds of the nose (middle and lower sections) if crooked will have to be addressed. This means addressing the upper and lower cartilages (reorientation of the tip cartilages in the latter case) which may be asymmetrical therefore sutures, trimming, or grafts may be used and septal cartilage which may need to be repositioned by detaching it off the nasal floor. There's a difference between simply straightening a deviated septum (septoplasty) by chiseling out the hump &/or protruding side cartilage/bone for improved breathing vs straightening a crooked/twisted or slanted nose (a very challenging & complex task) which extends the length of the nose (septorhinoplasty). I plan on discussing this on a future post.
Sources:
Facial Plastic and reconstructive surgery by Ira Papel
Functional Reconstructive Nasal surgery by E.H. Huising & John A.M. DeGroot
Recommended Reading:
http://www.facialsurgery.com/ClkoffTPgt3_2011_05_01mh.html
http://emedicine.medscape.com/article/1292249-treatment#a1133
Video's:
http://www.youtube.com/watch?v=kWoAXKPZr-A&feature=related
http://www.youtube.com/watch?v=IiIDmOZmbec
©noserevisionsurgeryandsurgeons.blogspot.ca
Friday, June 22, 2012
Tragal cartilage graft: Another donor site for cartilage
Tragal cartilage graft is taken from the tragus region of the ear. Gubiesch and Kotzur in a three year study reported in 2003, using tragal cartilage grafts in 84 cases none experienced donor site morbidity. They were able to harvest grafts up to 1.5cm by 1.5 cm in size. The advantage of tragal cartilage over conchal cartilage is that it is flat and less elastic. The authors consider it, therefore, to be the ideal graft for augmentation of the dorsum, compensation of irregularities, or correction of open roof deformities. They also claim that the tragus is easily accessible, as a donor site. In another 2007 study Cochran and Defatta determined that the tragus provides a simple, convenient alternative source of cartilage for rhinoplasty in graft-depleted patients. Tragal cartilage grafts were used in three primary and three secondary
rhinoplasty patients. Postoperative follow-up ranged from six months to
12 months. Tragal cartilage was used as five alar contour grafts, one
lateral crural onlay graft, one dorsal onlay graft, and one infratip
lobule graft. Tragal cartilage was used to close the septal perforation
of one patient. Tragal contour was preserved in all patients, and there
were no complications noted with this procedure.
http://resources.metapress.com/pdf-preview.axd?code=nfdp7053vbm2ptp6&size=largest
http://www.sciencedirect.com/science/article/pii/S0194599807018037
One study did find a negative side effect to use of tragal cartilage removal. Pothier D.D & Charaklias N. in 2006 study showed ten of the 12 patients in the tragal harvesting group who had used " in the ear"earphones pre- and post-operatively had had problems with earphones post-operatively, which in eight cases were due to pain or the devices falling out. Of the 12 respondents in the non-tragus group, only one had similar problems (p<0.05).
http://www.ncbi.nlm.nih.gov/pubmed/16939664
©noserevisionsurgeryandsurgeons.blogspot.ca
http://resources.metapress.com/pdf-preview.axd?code=nfdp7053vbm2ptp6&size=largest
http://www.sciencedirect.com/science/article/pii/S0194599807018037
One study did find a negative side effect to use of tragal cartilage removal. Pothier D.D & Charaklias N. in 2006 study showed ten of the 12 patients in the tragal harvesting group who had used " in the ear"earphones pre- and post-operatively had had problems with earphones post-operatively, which in eight cases were due to pain or the devices falling out. Of the 12 respondents in the non-tragus group, only one had similar problems (p<0.05).
http://www.ncbi.nlm.nih.gov/pubmed/16939664
©noserevisionsurgeryandsurgeons.blogspot.ca
Thursday, June 21, 2012
Ethnic Noses: Rhinoplasty surgeons experienced in ethnic rhinoplasty
Rhinoplasty surgeons are striving to respect ethnic nasal variations realizing that patients typically want to refine their nasal appearance yet preserve their ethnic features. This respect serves to maintain facial harmony among the esthetic units and tends to achieve a natural look.
Rhinoplasty surgeons experienced in ethnic noses (African American, Asian, Hispanic & Middle Eastern noses):
Dr. Ferdinand A. Ofodile Plastic Surgeon cert. 1976
Dr. Jennifer Parker Porter E.N.T/Facial Plastics cert. 1998
Dr. Sam Rizk E.N.T/Facial Plastics cert. 2000
Dr. Oleh Slupchynski E.N.T/Facial Plastics cert. 1998
Dr. Jeffrey Epstein E.N.T/Facial Plastics cert. 1994
Dr. David Kim E.N.T/Facial Plastics cert. 2003
Dr. Sam Nacify E.N.T./Facial Plastics cert. 1999
Dr. Samuel Lam E.N.T./ Facial Plastics cert. 2002
Dr. Derek Kofi O Boahene E.N.T/Facial Plastics cert. 2005
Dr. Babak Azizzadeh E.N.T/Facial Plastics cert.2003
Dr. Monte Harris E.N.T/Facial Plastics cert.2000
Dr. Philip Young E.N.T/Facial Plastics cert.2005
Dr. Paul Nassif E.N.T/Facial Plastics cert. 1998
Recommended reading:
Chapter 13 Revision Rhinoplasty of the ethnic nose .Dr. Jennifer Parker Porter & Chapter 14 Asian Revision Rhinoplasty. Dr. Jeffrey M.Ahn & Dr. Jeffery C. Liu.
http://books.google.ca/books?id=4J95te00xY4C&pg=PA146&dq=asian+and+american+african+rhinoplasty&hl=en&sa=X&ei=9NXiT4LqKYKS2QX0kPm8Cw&ved=0CFkQ6AEwBg#v=onepage&q=asian%20and%20american%20african%20rhinoplasty&f=false
Race vs Ethnicty
http://www.diffen.com/difference/Ethnicity_vs_Race
©noserevisionsurgeryandsurgeons.blogspot.ca
Rhinoplasty surgeons experienced in ethnic noses (African American, Asian, Hispanic & Middle Eastern noses):
Dr. Ferdinand A. Ofodile Plastic Surgeon cert. 1976
Dr. Jennifer Parker Porter E.N.T/Facial Plastics cert. 1998
Dr. Sam Rizk E.N.T/Facial Plastics cert. 2000
Dr. Oleh Slupchynski E.N.T/Facial Plastics cert. 1998
Dr. Jeffrey Epstein E.N.T/Facial Plastics cert. 1994
Dr. David Kim E.N.T/Facial Plastics cert. 2003
Dr. Sam Nacify E.N.T./Facial Plastics cert. 1999
Dr. Samuel Lam E.N.T./ Facial Plastics cert. 2002
Dr. Derek Kofi O Boahene E.N.T/Facial Plastics cert. 2005
Dr. Babak Azizzadeh E.N.T/Facial Plastics cert.2003
Dr. Monte Harris E.N.T/Facial Plastics cert.2000
Dr. Philip Young E.N.T/Facial Plastics cert.2005
Dr. Paul Nassif E.N.T/Facial Plastics cert. 1998
Ethnic features: one nose does not fit all Dr. David W. Kim
Anatomical Variations
Disclaimer: it is overly simplistic to classify a non-Caucasian nose as an “ethnic” nose to which “ethnic rhinoplasty” principles apply. Two noses from two different ethnic backgrounds are likely to be as different from each other as they are from a Caucasian nose. In addition, significant variations in facial features are found within any given ethnic group. That being said, three broad nasal morphology types have been used to describe ethnic variations. The leptorrhine (“tall and thin”) nose is associated with Caucasian or Indo-European descent. Because it is the most extensively studied in modern nasal analysis, it also inevitably becomes the reference point for comparison when studying noses of different ethnicity's. Only recently have non-Caucasian standards of nasal analysis been developed for specific ethnic groups.
The platyrrhine (“broad and flat”) nose is associated with African
descent. It is characterized by thick skin, a low radix, a short dorsum,
a bulbous and underprojected tip, and flared nostrils. An analysis of
the African-American female nose shows that compared to the Caucasian
standard for nasal analysis, the columella-to-lobule ratio is decreased,
and the alar width relative to the intercanthal distance is increased. The mesorrhine (“intermediate”) nose has features intermediate between
the leptorrhine nose and the platyrrhine nose. The “typical” Asian or
Latino nose is commonly regarded as mesorrhine, with a low radix,
variable anterior dorsal projection, rounded and underprojected tip, and
rounded nostrils. In Dr. Kim’s practice, patients of different backgrounds tend not to
want to strive for measurements and metrics consistent with a Caucasian
leptorrhine nose. Rather, many patients prefer to soften certain
features of their nose while retaining some of their “ethnic identity”.
Recommended reading:
http://books.google.ca/books?id=4J95te00xY4C&pg=PA146&dq=asian+and+american+african+rhinoplasty&hl=en&sa=X&ei=9NXiT4LqKYKS2QX0kPm8Cw&ved=0CFkQ6AEwBg#v=onepage&q=asian%20and%20american%20african%20rhinoplasty&f=false
Race vs Ethnicty
http://www.diffen.com/difference/Ethnicity_vs_Race
©noserevisionsurgeryandsurgeons.blogspot.ca
Sunday, January 29, 2012
Does a narrowing of the nasal passage-way simply mean correcting the collapsed valve region with cartilage grafts?
After my second major nose revision which involved spreader cartilage grafts I ended up with unusual narrowing on my right nasal passage way. It was different then the valve collapse feeling I had experienced prior to this surgery back in 2001. I noticed by touch that the area of my passage way became much smaller; my natural septal cartilage slanted out towards the opening of the nostril (caudal septal deflection) and with a hand mirror I noticed a more slit like appearance further upwards. My nasal bridge is slanted slightly towards that side as well on visual inspection. But to my surprise every nose surgeon that I have seen claims my septum is fairly straight and what I need done is major grafting to support my nose due to nasal valve collapse. I always had some reservations about this as being all there was to it, however these surgeons reassure me that grafting helps you breath better so the nostrils don't close up with inward breathing. In 2005 I unfortunately had surgery with a young novice surgeon who claimed he knew how to fix my problem. He ended up putting very small pieces of cartilage on each side of my nose as a alar graft, however it only added to the problem. He apparently didn't make the grafts long and thick enough to make a measurable difference. Therefore it has only added weight to the region, and unfortunately he did a lot of reduction surgery which left me with host of other problems. Fast forward to today, i still have this narrowing on my right side which needs correcting. My right passage way is touching in certain regions in a stationary position (without breathing inward) throughout most of the day. I have seen a couple of examples of people online who claim after they had cartilage grafts done on their nose for nasal valve collapse they still didn't feel their breathing was much improved. So what is going on here? Of course it could be that the surgeon they had may not of done the surgery properly; the grafts may not be in right place or too large or small, or migrated after the surgery, etc. But what if there was another underlying problem that the nose surgeon didn't properly diagnose prior to surgery? I have thought about this because of my situation, and after coming across some information in my research , a couple things stood out.
In my post titled 'Surgical options for treating Internal nasal valve collapse obstruction" it discusses how surgeon can improve the cross sectional area (changing the internal valve angle) simply with Flaring Sutures or with Prolene Suspension sutures. It states that "although the spreader grafts moves the dorsal border of the upper lateral cartilage in a lateral direction, the angle of the Internal valve is minimally affected. That post also discusses outfracture osteotomy of the nasal bones to widen the valve angle. Occasionally severe valve narrowing occurs after rhinoplasty as a result of Lateral osteotomy with infracture. These patients can be treated with revision osteotomy with outfracture of the nasal bones to widen the valve angle. A change of 1 degree in valve angle increased the area by approx. 4mm2.
I started thinking about whether or not my previous surgeon in 2001 did an infracture osteotomy on me. Could this be a missing piece of the puzzle to explain at least partly my narrowing condition resulting from that surgery? So I looked back at my operative report from 2001 and low and behold an infracturing osteotomy was performed on my right side. It said "the nasal bones were deviated to the right and therefore bilateral piriform incisions were made with osteotomies and infracturing, with good alignment".
So whether or not cartilage grafting would be enough to resolve my problem is something I will have to question now being aware of this. This proves how important it is to have your operative reports and to understand them. There were other things in the report which I only recently realized were not done according to recommendations such as the size of the L strut left behind in my septum. So if you've had a failed rhinoplasty, and not sure or fully content you have received answers to why you ended up with the poor results you have, do yourself a favor read and reread your operative report and research the medical terminology for better understanding. Just a quick mention, here- sometimes reports don't mention everything that was performed in the surgery, but don't discount the reports either, they may explain exactly why you are experiencing the problems you now live with. I will discuss osteotomy's in greater detail in a future post.
http://emedicine.medscape.com/article/1292249-overview
©noserevisionsurgeryandsurgeons.blogspot.ca
In my post titled 'Surgical options for treating Internal nasal valve collapse obstruction" it discusses how surgeon can improve the cross sectional area (changing the internal valve angle) simply with Flaring Sutures or with Prolene Suspension sutures. It states that "although the spreader grafts moves the dorsal border of the upper lateral cartilage in a lateral direction, the angle of the Internal valve is minimally affected. That post also discusses outfracture osteotomy of the nasal bones to widen the valve angle. Occasionally severe valve narrowing occurs after rhinoplasty as a result of Lateral osteotomy with infracture. These patients can be treated with revision osteotomy with outfracture of the nasal bones to widen the valve angle. A change of 1 degree in valve angle increased the area by approx. 4mm2.
I started thinking about whether or not my previous surgeon in 2001 did an infracture osteotomy on me. Could this be a missing piece of the puzzle to explain at least partly my narrowing condition resulting from that surgery? So I looked back at my operative report from 2001 and low and behold an infracturing osteotomy was performed on my right side. It said "the nasal bones were deviated to the right and therefore bilateral piriform incisions were made with osteotomies and infracturing, with good alignment".
So whether or not cartilage grafting would be enough to resolve my problem is something I will have to question now being aware of this. This proves how important it is to have your operative reports and to understand them. There were other things in the report which I only recently realized were not done according to recommendations such as the size of the L strut left behind in my septum. So if you've had a failed rhinoplasty, and not sure or fully content you have received answers to why you ended up with the poor results you have, do yourself a favor read and reread your operative report and research the medical terminology for better understanding. Just a quick mention, here- sometimes reports don't mention everything that was performed in the surgery, but don't discount the reports either, they may explain exactly why you are experiencing the problems you now live with. I will discuss osteotomy's in greater detail in a future post.
http://emedicine.medscape.com/article/1292249-overview
©noserevisionsurgeryandsurgeons.blogspot.ca
Subscribe to:
Posts (Atom)